In healthcare, the integrity and reliability of medical supplies are paramount for ensuring patient safety and effective treatment outcomes. Understanding the shelf life of these supplies is crucial, as it directly influences their functionality and safety. From disposable gloves to durable medical equipment, each category of medical supply has its specific lifespan, governed by various factors, including material composition, storage conditions, and regulatory standards. This article explores the longevity of different medical supplies, shedding light on how healthcare providers can manage these resources to maintain the highest standards of care. As the healthcare industry continues to evolve, so does the importance of resource management, making it imperative for professionals to stay informed about the best practices for medical supply longevity.
Contents
Understanding the Shelf Life of Medical Supplies
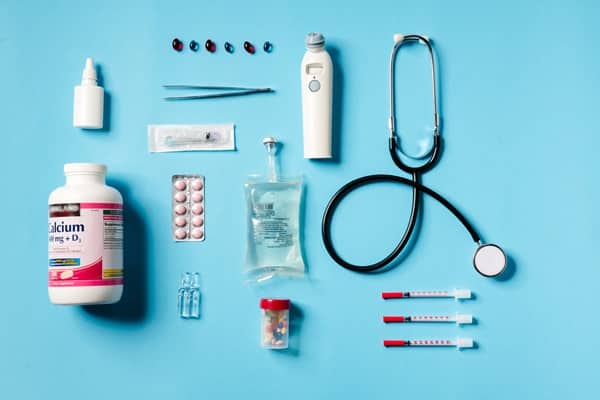
The concept of shelf life in medical supplies encompasses the duration these items remain safe and effective. This period is determined by manufacturers based on rigorous testing and regulatory guidelines, considering factors such as material degradation, potential for contamination, and efficiency loss over time. Understanding these timelines is essential for healthcare providers to ensure that they are utilizing supplies within their optimal performance period, thereby safeguarding patient care standards.
Moreover, the shelf life of medical supplies is not a static attribute but can be influenced by external conditions such as exposure to sunlight, temperature fluctuations, and humidity. This variability necessitates a proactive approach from healthcare facilities in managing their inventories, ensuring that supplies are stored under conditions that preserve their integrity. By adhering to best practices in storage and rotation, healthcare providers can minimize waste and avoid the risks associated with using degraded supplies.
The Variability of Shelf Life Among Different Medical Supplies
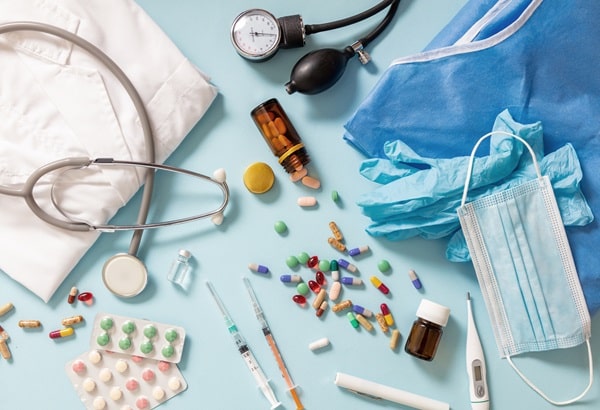
Not all medical supplies are created equal when it comes to shelf life. Disposable items like syringes and gloves often have a shorter shelf life than durable medical equipment like stethoscopes and hospital beds. This distinction is largely due to the materials used in manufacturing and the intended use of the supplies. Disposables are designed for single use to prevent cross-contamination, whereas durable items are built to last longer and withstand repeated use.
Understanding this variability is crucial for effective inventory management in healthcare settings. It requires a tailored approach to each supply category, with stringent monitoring of expiration dates for disposables and regular maintenance checks for durable equipment. This differentiation ensures that all medical supplies are used within their effective lifespan, maximizing patient safety and the overall efficiency of healthcare delivery.
Factors Influencing the Shelf Life of Medical Supplies
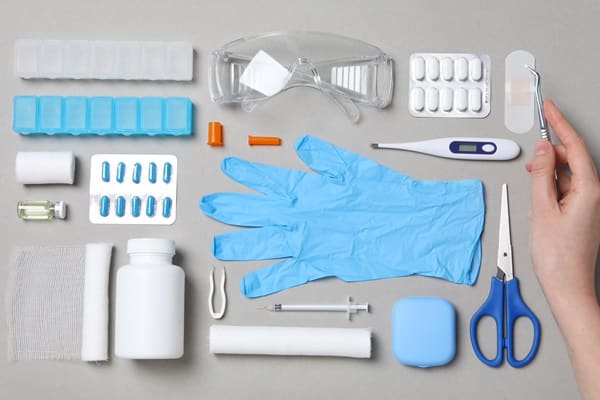
Several factors play a critical role in determining the shelf life of medical supplies. First and foremost, the material composition of an item can significantly affect its durability and susceptibility to degradation. For example, rubber and latex products may deteriorate over time due to oxidation, while metal components in medical equipment may be prone to corrosion if not properly maintained.
Storage conditions are another pivotal factor, as extreme temperatures, moisture, and exposure to light can accelerate the deterioration of sensitive medical supplies. Pharmaceuticals, in particular, require controlled environments to maintain their efficacy. Consequently, healthcare facilities must invest in appropriate storage solutions and adhere to recommended guidelines to preserve the quality and safety of their medical supplies.
The Impact of Regulatory Standards on Shelf Life

Regulatory agencies, such as the Food and Drug Administration (FDA) in the United States, establish stringent standards for the shelf life of medical supplies. These standards ensure that products reaching patients are safe, effective, and of the highest quality. Manufacturers must conduct stability testing as part of the regulatory approval process, determining how long their products can be expected to perform as intended.
Compliance with these regulations is a legal requirement and a critical component of patient safety. Healthcare providers rely on these standards to guide their inventory management practices, ensuring that all medical supplies used in their facilities meet the established criteria for shelf life. This regulatory oversight also facilitates continuous improvement in manufacturing processes, driving innovation in materials and preservation techniques to extend the shelf life of medical supplies.